A
63 year old male with a long standing history of hypertension, hyperlipidemia
and long standing tobacco abuse presents to the emergency room with a four
hour complaint of severe chest pain, nausea, dyspnea and diaphoresis.
On examination, the patient is in moderate distress. His skin is warm and
dry. BP is 95/60 mm Hg and pulse is regular at 70/min. Neck veins are 4
cm above the clavicle at 30 degrees but there is no abdomino-jugular reflux
There is an S4 gallop at the apex together with a grade 2/6 systolic ejection
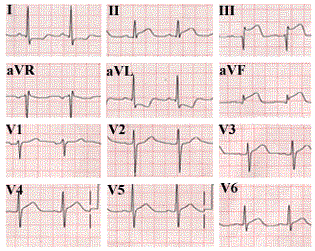
murmur. Lungs are clear and the peripheral pulses are normal. His ECG is
shown, below.
The patient received sublingual NTG, 3 mg of intravenous morphine sulfate,
and ASA gr. V. Two minutes later, the patient's BP drops to 70/30 mm Hg.
Pulse is 60/min. |